Living with persistent knee pain can be frustrating, especially when it starts affecting your daily routine, independence, and peace of mind. When knee pain becomes severe, long-lasting, and unresponsive to medications, physiotherapy, or injections, many patients are advised to consider Total Knee Replacement Surgery. However, before any decision is made, a detailed knee replacement consultation is the most important first step.
Many patients feel anxious before meeting the surgeon because they do not know what the consultation involves. This page explains in detail what happens during a total knee replacement consultation, what doctors assess, what tests are done, what questions patients should ask, and how this consultation helps in making the right decision confidently.
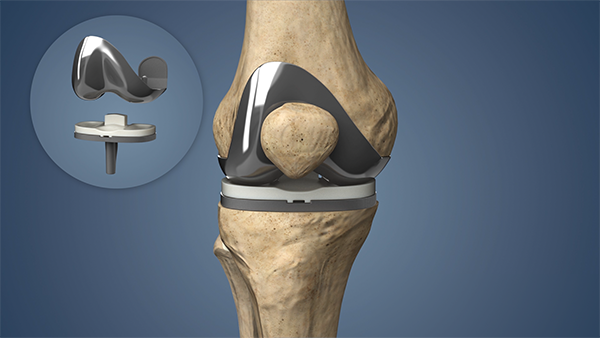
Understanding the Purpose of a Knee Replacement Consultation
The primary aim of the consultation is not to push you immediately into surgery. Instead, it is to:
Understand your knee problem in detail
Identify the exact cause of your pain and disability
Assess whether you truly need surgery
Explore whether non-surgical options may still work
Evaluate if you are medically fit for surgery
Help you understand what to expect from treatment
Plan the best personalized treatment strategy for you
The consultation ensures that you receive the safest, most appropriate, and most effective treatment, tailored to your health, lifestyle, and expectations.
Step 1 — Detailed Discussion About Symptoms and Medical History
Your consultation usually begins with a detailed conversation. The surgeon will talk to you to understand:
✔️ Nature of Your Knee Pain
How long have you been experiencing pain?
Is the pain constant or occasional?
Where exactly is the pain located?
Does it worsen while walking, climbing stairs, standing, or resting?
Does it disturb your sleep?
This helps determine the severity and impact of your knee condition.
✔️ Effect on Daily Activities
You will be asked about how knee pain affects your daily life:
Do you have difficulty walking?
Do you struggle to climb stairs?
Are you unable to sit cross-legged or squat?
Do you need support while walking?
Has your mobility decreased significantly?
If pain is affecting your quality of life and freedom of movement, it becomes a key consideration.
✔️ Previous Treatments Tried
Your surgeon will review all previous treatments, including:
Pain relief medications
Physiotherapy or exercises
Steroid or gel (viscosupplementation) injections
Knee braces
Weight management attempts
If these treatments have been tried consistently and have failed to provide relief, surgery becomes a stronger consideration.
✔️ Medical Background
The doctor will also ask about:
Diabetes
Blood pressure
Heart conditions
Kidney problems
Previous surgeries
Allergies
Medications currently taken
History of blood clots
Smoking or alcohol history
These details help ensure safety and medical readiness.
Step 2 — Physical Examination of the Knee
After the discussion, the surgeon performs a thorough physical examination. This helps assess:
🔹 Knee Alignment
Checking whether your knee alignment is normal or affected by deformities like:
Bow legs (Varus deformity)
Knock knees (Valgus deformity)
🔹 Range of Motion
The surgeon checks:
How much your knee can bend
How much your knee can straighten
Whether it feels stiff
Whether movement causes pain
🔹 Joint Stability
Doctors examine:
Whether the knee feels unstable
Whether it gives way while walking
Strength of supporting muscles and ligaments
🔹 Swelling and Tenderness
Signs of inflammation, fluid accumulation, and tenderness indicate severity of arthritis.
🔹 Walking Pattern (Gait)
The surgeon may ask you to walk a few steps to observe:
Limping
Movement restriction
Weight bearing discomfort
This physical examination gives important real-time information.
Step 3 — X-Rays and Imaging Studies
Medical imaging plays a crucial role in evaluating knee damage. During the consultation, your surgeon may request:
✔️ X-Rays
They help assess:
Joint space reduction
Bone damage
Arthritis severity
Deformity extent
Bone alignment
Joint wear and tear
X-rays are the most important imaging tool for knee replacement planning.
✔️ MRI (If Required)
MRI may be recommended in some cases to study soft tissues, ligaments, cartilage condition, or complex structural issues.
✔️ Blood Tests (Pre-Evaluation)
Sometimes preliminary blood tests may be advised to:
Check infection risk
Assess general health
Evaluate readiness for surgery
Step 4 — Understanding Whether You Truly Need Surgery
A good knee replacement consultation is honest, transparent, and medically justified. After evaluating your condition, your doctor may conclude one of the following:
🟢 You Need Knee Replacement Surgery Soon
This decision is taken if you have:
Severe pain
Advanced arthritis
Structural joint damage
Major mobility limitations
Failure of non-surgical treatments
In such cases, surgery is the most reliable solution for long-term relief and mobility restoration.
🟡 Surgery May Be Needed Later
If arthritis is moderate or symptoms are tolerable, your doctor may suggest:
Weight reduction
Physiotherapy
Lifestyle modifications
Medication support
Regular monitoring
This approach helps slow down progression.
🔵 Surgery Not Required
If your condition is mild or manageable, your doctor may advise conservative treatment instead of surgery.
A responsible consultation ensures surgery is recommended only when truly necessary.
Step 5 — Explanation of Treatment Options
If knee replacement is recommended, the doctor will clearly explain:
Why surgery is necessary
What happens during the procedure
Type of implant suitable
Robotic or conventional options (if applicable)
Expected benefits
Limitations
Long-term expectations
This helps patients make an informed decision.
Step 6 — Discussing Risks and Safety Measures
Every surgery has risks, but knee replacement is one of the safest orthopedic procedures worldwide. During consultation, patients are informed about possible risks such as:
Infection
Blood clots
Stiffness
Implant wear
Rare complications
Doctors also explain how these risks are minimized through:
Advanced surgical technology
Sterile protocols
Antibiotics
Preventive medications
Expert post-operative care
Step 7 — Understanding Recovery and Rehabilitation
Patients often worry about recovery time. During consultation, doctors explain:
📌 Hospital Stay
Usually 2–4 days depending on condition.
📌 Pain Control
Modern anesthesia and medications ensure comfortable recovery.
📌 Walking After Surgery
Most patients begin standing and walking within 24–48 hours with assistance.
📌 Physiotherapy
Essential for:
Strength building
Knee movement improvement
Faster recovery
Return to normal activity
📌 Return to Daily Life
With proper rehabilitation, patients can:
Walk comfortably
Climb stairs
Travel
Resume normal routines
within a guided time frame.
Step 8 — Financial and Practical Discussion
Depending on the hospital system, consultation may also include:
Surgery cost explanation
Insurance/cashless options
Hospital packages
Length of hospital stay
Follow-up visits plan
Clarity helps reduce unnecessary stress.
Step 9 — Personalizing the Decision
Every patient is unique, and knee replacement is not just a medical decision but also a life decision. Doctors consider:
Your age
Lifestyle needs
Work demands
Activity expectations
Family support
Personal preferences
This ensures you receive care that truly suits your life.
Frequently Asked Questions
1. What happens during a total knee replacement consultation?
The doctor reviews your symptoms, medical history, performs a knee examination, and evaluates X-rays or MRI to decide whether surgery is required.
2. Do I need to bring previous medical reports to the consultation?
Yes. Bring previous X-rays, MRI scans, medical history, medication list, and any previous treatment records for accurate assessment.
3. Will surgery be decided immediately during the consultation?
Not always. Surgery is recommended only when pain is severe, knee damage is advanced, and conservative treatments have failed.
4. Will the doctor explain different treatment options?
Yes. The doctor explains whether surgery is needed, available techniques, implant options, recovery expectations, and long-term outcomes.
5. Do I need X-rays or MRI before consultation?
If you already have recent knee X-rays or MRI, bring them. If not, the doctor may suggest imaging during or after consultation.
6. Will recovery and rehabilitation be discussed?
Yes. The doctor explains hospital stay, walking timeline, physiotherapy plan, recovery duration, and when you can return to normal activities.
7. Are risks and safety of knee replacement explained?
Absolutely. The doctor discusses possible risks like infection, stiffness, clots, and how advanced techniques reduce these risks.
8. How long does a knee replacement consultation take?
A detailed consultation usually takes around 20–40 minutes depending on examination, imaging, and discussion.
9. Will I get cost and insurance information during consultation?
Yes. Most hospitals provide cost, insurance, and package details during or after the consultation.
10. What is the main goal of a knee replacement consultation?
The main goal is to understand your condition, confirm whether surgery is needed, plan safe treatment, and help you make an informed decision.
Table of Contents
Total knee replacement surgery is a procedure in which damaged knee joint surfaces are replaced with artificial components to relieve pain and improve movement. Total Knee Replacement
Total knee replacement is suitable for individuals with severe knee pain, stiffness, and joint damage that no longer improves with medications, injections, or physiotherapy. Candidates
The cost of total knee replacement varies based on implant type, surgical technique, hospital stay, and rehabilitation requirements, so an individualized evaluation is essential. Cost
Patients should ask about the necessity of surgery, procedure details, implant type, benefits, risks, hospital stay, recovery time, rehabilitation, and long-term expectations — Questions to Ask.
Total knee replacement is generally safe and highly successful, though complications like infection, bleeding, blood clots, stiffness, or implant wear may rarely occur, which can be minimized with expert care — Risks and Safety.
Preparation includes medical evaluation, medication review, pre-surgery exercises, home planning, and understanding the procedure and recovery process. Preparation
The procedure involves removing damaged joint surfaces, placing artificial components, restoring alignment, and closing the joint with postoperative care. Steps
Recovery typically includes pain control, early mobilization, physiotherapy, gradual strength improvement, and regular follow-up visits. Recovery
Most patients experience significant pain relief, improved knee function, better mobility, and enhanced quality of daily activities. Results
Before-and-after results often show reduced pain, improved joint alignment, increased walking ability, and better overall knee movement. Before and after
Choosing the right surgeon involves assessing experience, specialization in joint replacement, patient outcomes, and clear communication. Choosing the right surgeon
